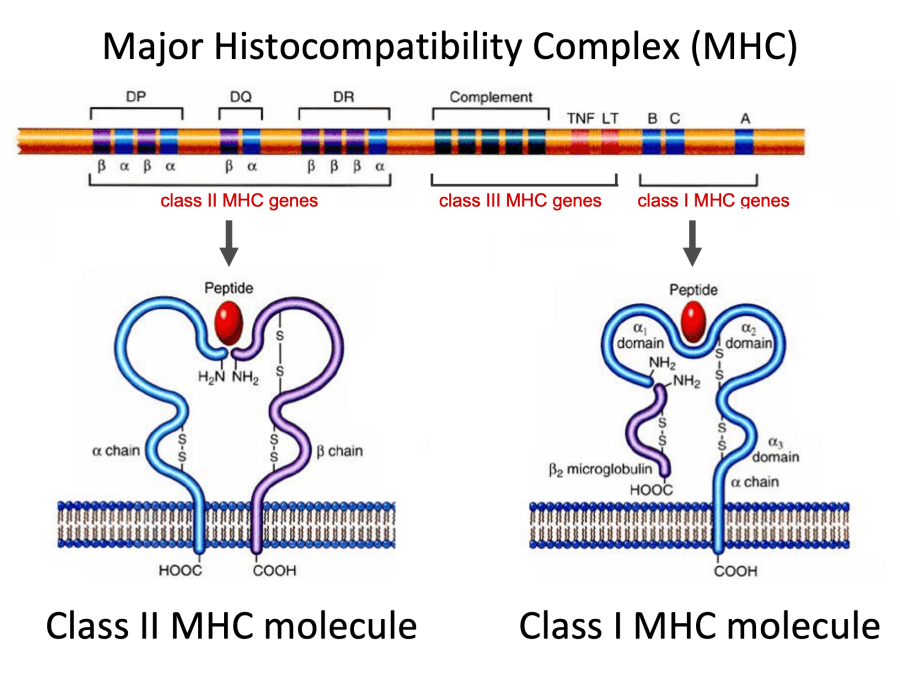
We talked a little bit about MHC I and II receptors in our Immunology Overview lecture. I intentionally kept our discussion pretty basic, because my goal in this lecture is just to get you up to speed with concepts you’ll need to understand for later lectures.
But there are so many things about MHC receptors and genes that can be confusing – and I wanted to share some things with you that took me a long time to understand, just in case you have the same questions.
For example, I was confused as a med student as to what each MHC gene produced. Okay, so there are three class I MHC genes (A, B, and C). Does each of gene encode a particular part of the MHC class I molecule?
Turns out, the answer is no! Each gene (A, B, and C) encodes an ENTIRE MHC I molecule.
Okay…so there are three different class I molecules on all my cells? No – there are 6 (because you have two major histocompatibility complexes – one on each chromosome 6).
If you have questions like these, you might find these two posts helpful:
Please note that this is just optional reading!! For our quizzes and exam, you are ONLY responsible for the material we cover in lecture. When I write test questions, I focus on the material in the learning objectives, and I don’t ask about anything that isn’t in the lecture slides.
But I like to share things that took me forever to figure out, because it might save you guys time.