Venus Williams announced she had Sjogren’s syndrome back in 2011. She discusses her experiences with the disease in this YouTube video as well as this CNN interview. She is most definitely not letting the disease define her. She just hosted this year’s Met Gala and is as gorgeous and strong as ever.
What’s it like to have scleroderma?
Tomorrow we’ll talk about the systemic sclerosis, or scleroderma.
The New York Times has a nice recurring feature called “Patient Voices” in which several patients with a particular disease talk about how that disease has affected their lives. Here is a Patient Voice article on scleroderma. It’s a bunch of short stories (a couple minutes each), narrated by the patients themselves, accompanied by a series of photos of the patient. I highly recommend you listen to some of these. I identified with “The Mom with Frozen Fingers;” you may wish to start with “Losing his color” which is narrated by a 26 year old man. I think you’ll probably find yourself listening to more than one.
There are others Patient Voices segments on lupus and Sjogren syndrome too.
Selena Gomez and others talk about lupus
Selena Gomez has been battling lupus for many years. She’s been open about her diagnosis and has talked very candidly about the toll it’s taken on her.
Here are some articles and videos, if you want to read/watch more:
- She has a documentary called “My Mind and Me” on Apple TV. Here’s a short trailer.
- Here’s a fairly recent Today Show article/video in which she talks about her health.
- Here is an older ABC article in which Selena and other patients talk about what it is really like to have lupus.
In 2017, she underwent a kidney transplant for complications related to her disease. Her disease course is more severe than it is for many patients with the disease; kidney transplants are typically used only after other, less dangerous treatments fail.
Quiz 2 information
As I mentioned last week, tomorrow’s Quiz 2 will NOT be given in class!
It is a take-home, open-book, talk-with-each-other if you want quiz, posted on Canvas. It has 10 multiple-choice, single-answer questions, each worth 1 point, and it covers all the lecture material from 5/27 through and including the slides we will cover today.
It will be open from Monday, June 8 at noon until Wednesday, June 10 at 11:59 pm. You can take the quiz at any time during that period.
You’ll have 20 minutes to complete it once you start (people with accommodations have time adjusted accordingly). Please complete and submit it by 11:59 pm Wednesday.
Any questions, let me know!
Schedule tweak for Monday, June 8
We’ve been doing some in-class Kahoot questions, no-stakes, no points, just to reinforce the points I want to make sure I get across to you. And you guys have been doing REALLY WELL, I just want to say! It’s impressive 🙂
Adding in those Kahoot questions has been good, I think – but it also takes up a part of our lecture time, and we’re just a little behind (we got through most of Autoimmune diseases today, but there are still 10 slides left).
In order to keep our schedule organized and on time, I’d like to finish the rest of the Autoimmune Diseases slides on Monday, June 8, then go through a few in-class Kahoot questions on Autoimmune Diseases, and then turn Quiz 2 into a take-home, open-book quiz. I’m going to see how the Canvas quiz options work – and if that seems like a good option, we’ll use that platform. Otherwise, I’ll use Google forms.
That way we’ll be on track to do Transfusion Medicine on Wednesday without missing anything.
By the way, I’ve been posting the short in-class Kahoots both on our Kahoots page and on our Schedule page, in case you want to go back and look at them.
Please let me know if you have any questions!
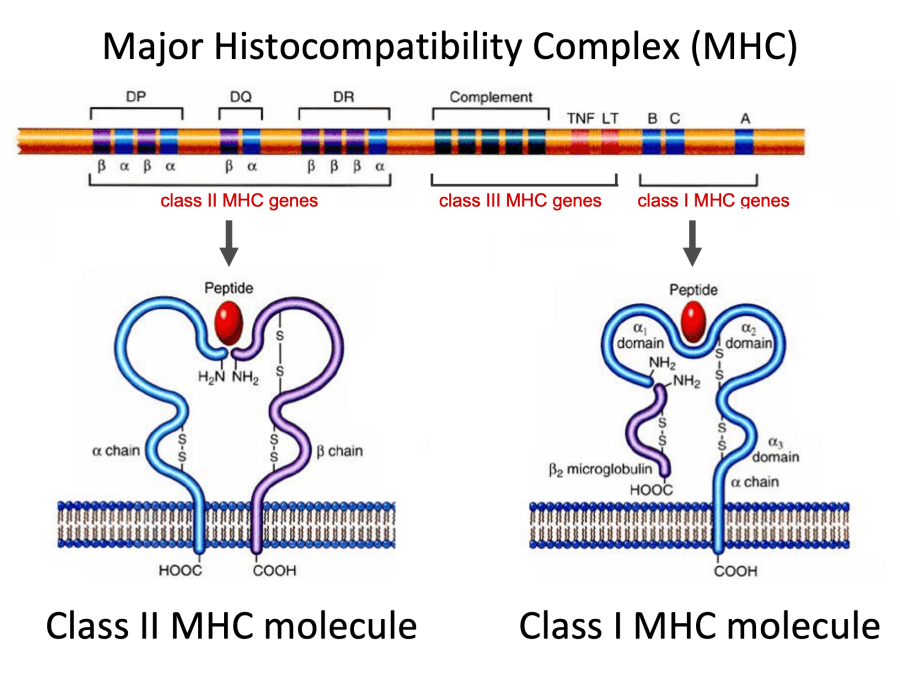
MHC receptors and genes can be confusing
We talked a little bit about MHC I and II receptors in our Immunology Overview lecture. I intentionally kept our discussion pretty basic, because my goal in this lecture is just to get you up to speed with concepts you’ll need to understand for later lectures.
But there are so many things about MHC receptors and genes that can be confusing – and I wanted to share some things with you that took me a long time to understand, just in case you have the same questions.
For example, I was confused as a med student as to what each MHC gene produced. Okay, so there are three class I MHC genes (A, B, and C). Does each of gene encode a particular part of the MHC class I molecule?
Turns out, the answer is no! Each gene (A, B, and C) encodes an ENTIRE MHC I molecule.
Okay…so there are three different class I molecules on all my cells? No – there are 6 (because you have two major histocompatibility complexes – one on each chromosome 6).
If you have questions like these, you might find these two posts helpful:
Please note that this is just optional reading!! For our quizzes and exam, you are ONLY responsible for the material we cover in lecture. When I write test questions, I focus on the material in the learning objectives, and I don’t ask about anything that isn’t in the lecture slides.
But I like to share things that took me forever to figure out, because it might save you guys time.
Excuse me, may I smell your MHCs?
Check out this interesting concept. You already know that the MHC I receptor is present on (pretty much) every cell in the body and presents antigen to cytotoxic T cells, and that the MHC II receptor is present only on specialized antigen-presenting cells and presents antigen to helper T cells. Right.
But did you know that these same receptors may be helping a woman decide on a mate? It seems that women prefer mates with MHCs very different from their own. That seems like a good idea – it helps provide diversity within the genome.
It would be hard to get a sample from every guy and bring it to the HLA-typing lab, but no need: the brain can detect MHC differences by smell (they’re associated with pheromones)! Weird. And cool.
So what are the in-class Kahoot quizzes like?
I’ve gotten a few emails asking about the format of the Kahoot quiz tomorrow, and I thought I’d post my answers to the whole class.
The quizzes in this course are given in the classroom using Kahoot, just like we did in our last class session, when I used Kahoot to ask you about stuff we just talked about.
By the way, did you guys find those no-stakes Kahoot questions useful? I’d really really appreciate it if you could take a sec and just answer this question yes or no, so I can decide whether to keep doing it.
I’ll give you a minute to answer each question, and you can use your notes/lecture slides, and talk to each other (sometimes that’s a good way to learn!) during the quiz. There will be 10 multiple-choice questions, each worth one point.
These points will just sit in your points bank, and at the end of the course, I’ll add up all your points for the quizzes and exam to get a final point total, which is what I’ll use to determine your grade (you can read more about grading here). No weighting of quizzes/exam, and no curving. Just straight up 90% (or more) of total possible course points = A, 80% or more = B, etc.
If you have accommodations, I will be sending you the Kahoot to complete on your own (with the appropriate time extension). I can see the accommodations list on the faculty intranet – but if you’re wondering if I know about your accommodations, just send me a quick email tonight to be safe.
If you have any more questions about how the quizzes work, let me know. I mostly want these to be learning opportunities (which is why I let you talk to each other) and a way to get more points into the course so your entire grade doesn’t rest on just the final.
What I like about you (part 1)
You guys are amazing, and I think you need someone to point that out to you in specific ways.
Here are two things that happened today:
1. Someone actually chased me down (apparently I walk very fast) to make sure I got my phone, which I left on the podium.
This is an example of compassion, and not just the “there, there” compassion, but the going out of your way type of compassion that inconveniences you but really helps the person on the other end. This is why I have such confidence in your ability to be wonderful healthcare providers.
You’re all smart, okay? Let’s get that out of the way. But do you care about others? YES!! You do, and it shows. Thank you, kind person 🙂
2. When I asked you if you’d like to end class at 12:00 rather than our official 12:05 stop time, you were honest and nodded your heads yes.
GREAT! Now I know, and I’ve gone in and changed all our end times to 12:00. I will honor that and finish on time so you get your break to stop thinking about this stuff for a moment and regenerate your willingness to sit and learn.
The lecture video for today is posted on our schedule page, and it should be playable.
Someone (again, thank you) was kind enough to tell me that the videos I posted for our first lectures were not visible to you guys.
They changed the settings in Mediasite this year so that I need to now need to go in and make sure the permissions are set correctly. Not a big deal, but it was something new this year that I didn’t realize had changed. So thanks for letting me know.
Please continue to give me feedback in real time like this! Otherwise, you will just sit and suffer, and life is too short for that.
Couple little summaries of cell injury plus a request
I mentioned yesterday that I have a website totally separate from our school websites that I run on my own – it’s called PathologyStudent.com and I actually use a lot of the questions I get from you guys as prompts for writing posts! So you might find something useful there.
Please, hear me on this: this is another totally optional resource. You have an extremely full schedule, and I want to offer you resources but also clarify that these are all just for your personal use, and there will not be anything on the exam that is not discussed specifically in class.
Here are a couple posts from Pathology Student related to cell injury:
- What’s going on inside a cell when it gets injured? (very quick review)
- A quick review of cell injury (also quick, but a few more details)
I really appreciate your feedback from the first day of class (the Kahoot we did) – and am still sorting through all the comments.
I would LOVE to hear more ideas from you guys on what I can do to make things better/easier/less stressful in this course. I can think of stuff from my end, but that’s not NEARLY as useful as getting suggestions from you.
Here’s a quick way to give me your thoughts – it’s just an anonymous Google form with a single open-ended question. I’d love to hear what you think now, so I can make important changes at the beginning of the course.